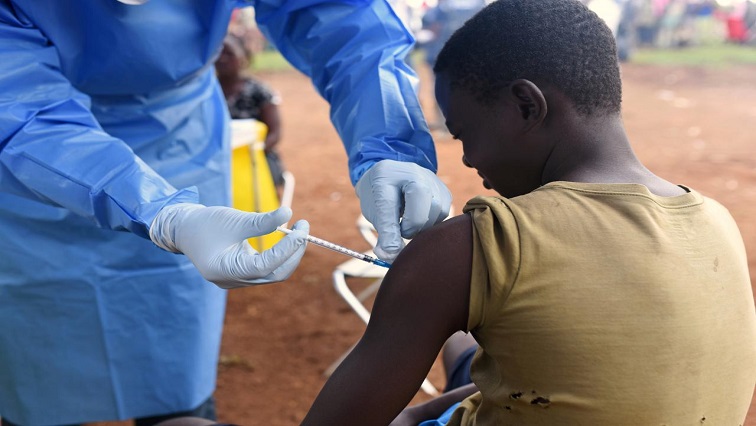
A quarter of people surveyed in Democratic Republic of Congo’s Ebola hotspots believed the virus was not real, a study said on Wednesday, as the world’s second-biggest outbreak spreads.
Health workers said public mistrust is now the biggest obstacle to stopping the epidemic, which has infected more than 1,000 people in eastern Congo since July, with many refusing vaccines, resisting treatment and concealing symptoms.
Harvard University researchers found that trust in public authorities had already fallen in the cities of Beni and Butembo before Ebola hit, due to decades of conflict and poor governance.
“It’s been three years now that we saw a declining level of trust in those actors, and the Ebola crisis comes on top of that and accelerates the distrust,” said Patrick Vinck, author of the study published in one of The Lancet’s speciality journals.
“In some ways, we are now paying the consequences of many years of lack of interest and focus on this issue,” he told the Thomson Reuters Foundation.
The world’s worst epidemic of Ebola, a haemorrhagic fever, killed more than 11,300 people in West Africa from 2013 to 2016.
The virus has infected 1,022 people and killed 639 in eastern Congo so far, according to the health ministry. In recent weeks, there has been on average eight new cases per day.
People who believed rumours that Ebola does not exist were 15 times less likely to seek formal health care and five timesless likely to accept vaccination, found The Lancet Infectious Diseases study, based on 961 interviews in September.
Local militias are active in the area and health workers are often accompanied by police and soldiers for security, which makes villagers suspicious, aid workers said. Ebola responders and centres have been targeted in numerous attacks.
December’s presidential election was cancelled in the affected areas, fuelling conspiracy theories.
Community resistance is highest in and around Butembo, the latest epicentre of the outbreak, said Jean-Philippe Marcoux,country director for international aid group Mercy Corps.
“We need to – as much as possible and rapidly – scale down the presence of security forces with response teams, because it is creating more harm than good right now,” he said.
Although the World Health Organization (WHO) and charitiesare running community engagement programmes, these have not been well-integrated with the medical response, Marcoux added.
But building trust is a slow process, said WHO’s regional emergencies director Ibrahima Soce Fall.
“What worked in Beni might not work in Butembo because the communities are not the same,” he said.